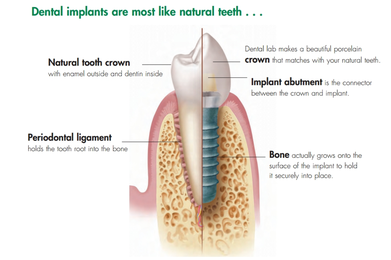
 A dental implant is one option to replace one, several or all of your missing teeth. Dr. Barroner works together with your other dental providers to help replace your missing teeth with dental implants so you can have a beautiful smile and continue to enjoy the food you love! A “dental implant” has several components: *the implant itself is medical grade titanium alloy that looks like a screw and takes the place of where your tooth root was. *the abutment is a part that screws into the implant which is what the crown or cap will be cemented or screwed onto (a healing abutment or healing cap is placed before the final abutment can be placed to allow for soft tissue healing). *the crown or “cap” fits on the abutment and is either screwed or cemented into place by your dentist, this is the part of the “dental implant” that you actually see above the gum tissue and looks like the white part of your tooth. Dental Implants can be useful in several situations: *Replacing a single tooth *Replacing several missing teeth with an implant supported bridge (uses two dental implants to support 2-4 teeth depending on the area) -Replacing all upper or lower teeth with multiple implants to support fixed (meaning the teeth stay in your mouth and can only be removed by your dental provider) or removable (dentures that snap onto implants to keep them in place) dental appliances 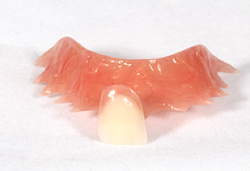 When can you have “teeth/caps” placed on the dental implants? This can vary depending on many factors such as the initial stability of the dental implant, location of the dental implant, health of the patient and patient’s bite but you could potentially have a temporary crown or denture placed the same day as the procedure. However, in many cases, the dental implant usually takes approximately 2-3 months to heal and fuse to your bone, after which point the implant will be ready to uncover (if it hasn’t been exposed already) and then restored with the crown/cap. If your dental implant can’t be restored right away your dentist can offer a temporary replacement that is usually removable. Some options include a “flipper” or an Essix retainer. Am I a candidate for a dental implant?
Dr. Barroner is pleased to offer complimentary implant consultations to determine if you a good candidate for dental implants. She will review your medical history and perform a clinical exam. In addition, in many cases Dr. Barroner may recommend a three dimensional x-ray called a Cone Beam CT (CBCT)* to further evaluate the hard and soft tissue structures which can affect implant treatment planning. *Please be advised additional fees may apply for the CBCT imaging. Written By: Dr. Meghan Barroner, D.M.D. 4/25/17
0 Comments
Depending on what type of procedure you are having and based on your health it may be recommended that you undergo some form of sedation or general anesthesia for your treatment. Our goal here at Elevated Oral & Implant Surgery it to provide the highest level of care for our patients and allowing them to have a positive, safe, comfortable experience. The more complex the surgery, or the more anxious you are about your upcoming treatment may be reasons to consider different types of anesthesia options. Dr. Barroner will discuss with you what type of anesthesia would be best for your particular situation.
Types of anesthesia: Local Anesthesia—this is what most people refer to as “Novocaine” or numbing medication. Regardless of whether or not you stay awake for your procedure we will always provide local anesthesia to help reduce any discomfort both during and after the procedure. Typically, this is the safest form of anesthesia, as any type of sedation carries some additional risk. We generally apply a topical numbing jelly before giving the local anesthetic injection, which helps make it more comfortable. The effects of the local anesthesia can be expected to last anywhere from 1-3 hours usually. Oral Sedation—with this form of sedation your doctor will prescribe an oral medication to take usually 1 hour before your scheduled treatment (and on occasion some patients will also be instructed to take this the night before the procedure as well). Most patients who opt for this type of sedation feel very relaxed, but are still usually aware of their surroundings and are not sleeping during the procedure, but everyone responds differently to the oral medication, so patients may have different experiences based on how the mediation affects them. You will not be permitted to drive yourself to or from the appointment if you have any form of sedation, including oral sedation, so you must have a responsible adult driver with you if you choose this type of anesthesia. Nitrous Oxide and Oxygen—this is commonly called “Laughing Gas”. This form of medication is a breathable gas that makes most people feel very relaxed, though similarly to oral sedation you generally are still aware of your surroundings, but just don’t care as much what is going on around you. This medication is also a very safe medication and due to its short acting duration, once we turn the gas off and you breath 100% oxygen after the treatment is complete the drug leaves your system quickly and you are safe to drive yourself home. IV Sedation and General Anesthesia—just as the name implies you will need to have an IV started for us to administer this type of sedation or anesthesia. This type of sedation puts most patients in a much deeper sleep than Oral Sedation or Laughing Gas, however some patients may have a brief period of time where they may wake up a bit and the doctor will administer additional medication to relax patients again (this allows the doctor to titrate the sedative medications for a safe and comfortable experience). This type of anesthesia does carry slightly more risk, but again your doctor will review if you are a good candidate for this type of anesthesia and discuss any possible risks with you and answer your questions prior to your treatment. There are special instructions you must follow for this type of anesthesia and they will be reviewed with you before your treatment. **For smaller children: Often times to perform treatment for anxious children utilizing some form of sedation is necessary for safe treatment and to help make their dental/oral surgery experience a non-traumatic one. Depending on your child’s weight the doctor may recommend an oral sedative medication which will generally allow them to cooperate well with the start of an IV. Also, depending on the level of anxiety and other factors the patient may do quite well with the laughing gas sedation. The doctor will discuss the recommended options for your child. Frequently Asked Questions: Who provides the Anesthesia? That is a great question! Oral & Maxillofacial Surgeons are a unique specialty and are the only practitioners aside from anesthesiologists that hold an unrestricted license to provide local anesthesia up to and including general anesthesia. We go through extensive anesthesia training during our hospital residency alongside of anesthesia residents that prepares us well to evaluate patients pre-operatively and provide safe anesthetic techniques tailored to each patients’ specific needs. We also have extensive training in rescue and resuscitation efforts should that ever be required. Our office is equip with all the necessary supplies to provide a safe and effective anesthetic. We are held to the same standards as an anesthesiologist would be when providing our anesthesia services. That being said, to answer the question of who provides the anesthesia---it is the Oral & Maxillofacial Surgeon who provides the anesthesia. Is the anesthesia safe? As mentioned previously all types of anesthesia carry some risk with them, even local anesthesia, but your doctor will review your medial history and clinical exam to determine your specific risks and determine what type of anesthesia would be best in your situation. Also, we often coordinate care with your other health care providers if needed to help minimize your anesthetic risks. Dr. Barroner carries up to date ACLS (advanced cardiac life support) and PALS (pediatric advanced life support) certificates and both she and her staff carry BLS/CPR (basic life support) certifications. They practice emergency drills to be prepared should any event arise. This is a great article to help you understand that our outpatient anesthesia services are very safe: http://www.aaoms.org/docs/govt_affairs/advocacy_white_papers/advocacy_office_based_anesthesia_whitepaper.pdf Written by: Meghan Barroner, D.M.D. 2/16/17 |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
POPULAR LINKS |
ADDRESSTelephone |
HoursMonday 9:30a-5:30p
(Summer hours on Monday: 8:00a-3:00p) Tuesday 8:00a-4:00p Wednesday 8:00a-4:00p Thursday 7:30a-3:30p Friday 7:30a-1:00p |
